Doctors Unite: Oregon’s Holistic Healthcare

For many U.S. citizens, scheduling a medical appointment raises a myriad of questions and decisions: What kind of specialist should I see? Is this practice affordable or in my insurance network? Will they know how to diagnose and treat my health issue? Some Oregon health professionals are taking revolutionary approaches to these questions in their practice and realizing the value of eclectic care. Together, doctors and therapists are teaming up under the same roof to provide affordable treatment while addressing the interconnectedness of physical and mental health.
The Physical vs. Mental Dichotomy
Here in the U.S., our healthcare system has become a highly specialized structure of professionals and referrals. Either a clinician will be able to address your needs, or pass you off to someone appropriately qualified. But St. Charles Health System in Bend, OR is trying something a step out of the ordinary: team-based care in which physicians and mental health specialists work side-by-side to more accurately diagnose and more effectively treat a variety of ailments. It requires no small amount of cooperation and synergy from professionals, but so far, the experiment’s results are promising.

There’s little doubt left in interpreting the relationship between physical and mental health, but implementation of these realizations are not yet up to speed with conclusive research. Physical health often takes priority, with symptoms more “real,” measurable, and threatening. In effect, the role of mental health has been vastly downplayed — even stigmatized. In the exam room of St. Charles, however, the psychologist enters no differently than the physician did, and helps bring a sense of normalcy to mental evaluations.
But how effective is this tandem of doctors compared to the traditional system of individual specialists? The success story of 17-year-old Tyson Engel, who suffered a concussion while snowboarding, hints that team-based care might be a viable model for future medical practice.
After experiencing headaches, loss of appetite, sleeplessness, and other strange behavioral symptoms, Tyson and his family turned to St. Charles for answers. Multiple visits to the ER and primary-care clinics failed to remedy Tyson’s symptoms, but in Bend, where a clinical psychologist works alongside a pediatrician, he began his upward climb to wellness.
The results were particularly surprising in that physical injuries are not often paired with mental health solutions. But in Tyson’s case, it made the difference that has practices across the U.S. wondering if they, too, should consider team-based care.
Prevalence of Mental Health Issues

As many as 1 in 5 Americans suffers a mental health disorder, but only about a third of those will seek professional help. National discussions surrounding mental health treatment have sparked across issues such as gun violence and drug addiction, but access to treatment remains narrow for many.
Cost isn’t the only factor driving people away from the care they need. A 2011 SAMHSA report uncovered the many different reasons why mental health is kept low priority:
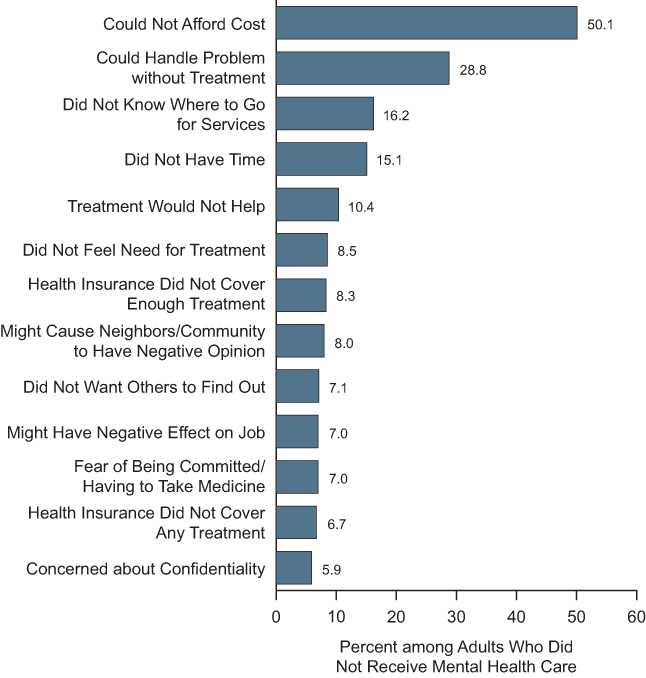
St. Charles' integrated team-based system challenges some of these reasons, but there’s still much work to be done in dissolving mental health’s stigma and increasing accessibility to treatment services.
Julie Hersh, author of Struck By Living: From Depression to Hope, describes this resistance: “Having seen numerous psychologists and psychiatrists, I believe one of the reasons people avoid the mental health system [is] because they see it as a quagmire of experts and medicine that often fails to get the job done.”
With fifty percent of Americans rejecting mental health treatment because of cost, accessibility remains a key discussion point.
In the case of Tyson Engel, learning new coping mechanisms from a psychologist made all the difference in his recovery. By demonstrating the importance and efficacy of mental treatment through team-based care, doctors will hopefully be able to turn these assumptions around.
Maximizing Resources
The political firefight of Obamacare has sparked controversy across the U.S. With fifty percent of Americans rejecting mental health treatment because of cost, accessibility remains a key discussion point. That’s why St. Charles is looking into how much a team-based model can save patients.
Current estimates say that Medicaid patients are saving an average $860 a year through collaborative practices, despite slight increases in pharmaceutical costs. According to analysts, the success and efficacy of team-based care is keeping people healthier longer and reducing the number of office visits per year.
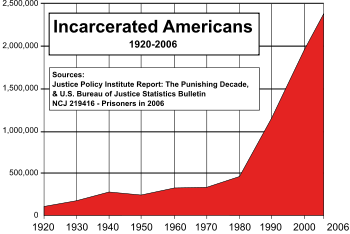
Less obvious are the dollars saved from eliminating social and criminal issues surrounding a need for more accessible mental health treatment. Incarceration costs have skyrocketed with overcrowded prisons, and with no resolution in sight. Studies show that mental health treatment greatly reduces the likelihood of an individual committing another criminal offense, making collaborative care a step in the right direction.
Upcoming studies based on St. Charles’ efficacy will reveal the practice’s true savings, but the long-term prospects are bright. More healthcare professionals are realizing the impact of psychology on the body and are adjusting their care plans accordingly. With more testing and research, Oregon’s team-based care could be the key to a happier, healthier society.
Sources
- http://www.npr.org/blogs/health/2013/10/22/226108057/doctors-enlist-therapists-to-deliver-better-cheaper-care
- http://thinkprogress.org/health/2013/10/23/2822801/oregon-mental-health-care/
- http://www.psychologytoday.com/blog/struck-living/201110/convincing-the-stubborn-accept-mental-health-care
- Photo Credit: SAMHSA, Incendant.com