Bridging the Treatment Gap

The 99%
Addiction is a disease which affects more Americans than heart conditions, diabetes or cancer, respectively. Forty million Americans ages twelve and older have an addiction involving nicotine, alcohol or other drugs; eighty million more are high-risk users, who are likely to harm themselves through future abuse (most Americans do not make a distinction between the two). Yet only 1% of all Americans receive successful intervention and addiction treatment. Why is it that 90% of Americans struggling with addiction receive no care at all?
Substance abuse and addiction are problems which affect men and women of all ages and socioeconomic levels, but successful treatment and recovery options are often only available for the wealthiest Americans. For everyone else, there is a strong reliance on public funds for addiction treatment: data from the 2008 National Household Survey on Drug Use and Health suggest that only about one-third (36%) of the individuals who received addiction treatment used private health insurance; the rest used savings (50%), Medicaid (25%), public assistance (22%), Medicare (18%), and family funds (17%).
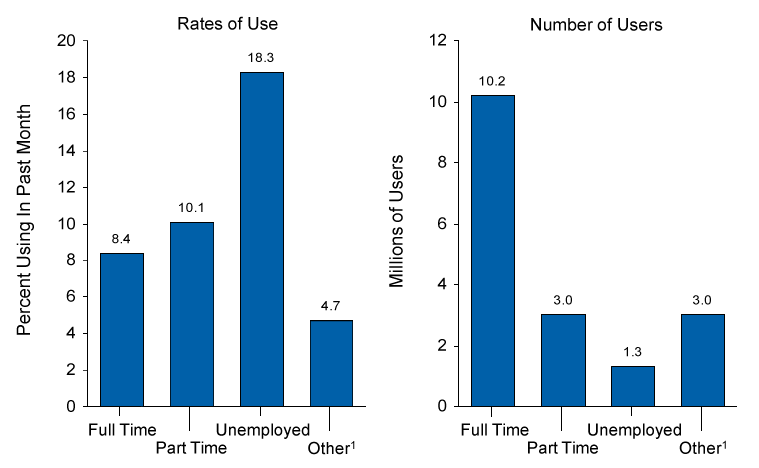
The treatment gap consists of a disproportionate amount of ethnic minorities, as well as unemployed adults and young adults aged 18 to 25 years. Both groups have limited access to health insurance and publicly funded addiction treatment services.
Is There a Doctor in the House?
Addiction treatment has been notoriously neglected by the United States medical system. Nearly half of all Americans say they would go to their healthcare providers if someone close to them was struggling with addiction, yet less than 6% of all referrals to addiction treatment come from health professionals. And only 29% of patients who had visited a medical provider were even asked about alcohol or other drug use in the past year. Misconceptions about the disease undermine proper medical care; while doctors routinely screen for a broad range of health problems like high blood pressure or high cholesterol, they rarely screen for risky substance use or signs of addiction. In fact, most medical professionals who should be providing treatment are not sufficiently trained to diagnose or treat addiction, while most of those providing addiction treatment are not required to have any medical training and are not equipped with the knowledge, skills or credentials necessary to provide the full range of evidence-based services. There are no accepted national standards for addiction screening, and requirements vary drastically from state to state.
 Americans are ahead of policymakers in their ability to grasp the complex nature of addiction and the value of addiction treatment services: seven of ten Americans (71%) consider alcohol and drug addiction to be a serious problem and 77% support efforts to make treatment more affordable and accessible. Addiction constitutes the largest preventable and most costly health problems facing America today, responsible for more than 20% of deaths in the U.S., causing or contributing to more than 70 other conditions requiring medical care and a wide range of costly social consequences and accounting for one-third of all hospital inpatient costs. Effective health care interventions to prevent and treat addiction would reduce these costs.
Americans are ahead of policymakers in their ability to grasp the complex nature of addiction and the value of addiction treatment services: seven of ten Americans (71%) consider alcohol and drug addiction to be a serious problem and 77% support efforts to make treatment more affordable and accessible. Addiction constitutes the largest preventable and most costly health problems facing America today, responsible for more than 20% of deaths in the U.S., causing or contributing to more than 70 other conditions requiring medical care and a wide range of costly social consequences and accounting for one-third of all hospital inpatient costs. Effective health care interventions to prevent and treat addiction would reduce these costs.
A New Hope
“It is time for health care practice to catch up with the science. Failure to do so causes untold human suffering and is a wasteful misuse of taxpayer dollars.” -Susan Foster, Vice President and Director of Policy Research and Analysis at CASA Columbia
Our knowledge of the science of addiction is growing, as well as our ability to identify the disease and intervene effectively. The current treatment benchmark for addiction disorders is outlined in a report from the healthcare nonprofit National Quality Forum which describes the 11 science and consensus-based treatment interventions relevant to the identification, assessment, intervention and continuing care components of treatment. Policymakers and legislators are beginning to understand the benefits of bridging the treatment gap as well.
In 2008, the Open Society Institute initiated a national program to expand access to, and funding for, drug and alcohol addiction treatment. The initiative aimed to mobilize public support for expanded treatment through three broad strategies:
- expanding insurance coverage
- increasing public funding
- achieving greater program and system efficiency
In 2010, two pieces of federal health care reform legislation, the Patient Protection and Affordable Care Act and the Reconciliation Act, provided health insurance for 32 million of the estimated 45 million uninsured people in the US through a combination of required, subsidized insurance and Medicaid expansion plans.
The combination of public support, health insurance coverage, and increased knowledge of treatment offers a unique opportunity to reduce disparities in access to and quality of treatment for addiction, but continued efforts to close the treatment gap and curb the impact of addiction on low-income communities should continue to be guided by sound research and practice. Integrating addiction treatment services into standard insurance policies and mainstream medical practice can be facilitated by technology and reinforced through structural relationships between care providers. As always, care should be safe, effective, timely, patient-centered, efficient and equitable.
“Finally, technology is key to communicating results and follow up to both patient and provider.” -Victor Capoccia, Director of the Closing the Treatment Gap program at the Open Society Institute
Of course, technology can also be used to raise awareness of issues and to find treatment and recovery options. If you or a loved one is suffering from drug or alcohol addiction, take the first step and call 1-877-822-7504 now for a free assessment.
Resources:
- http://www.drugabuse.gov/publications/drugfacts/nationwide-trends
- http://www.spotlightonpoverty.org/ExclusiveCommentary.aspx?id=049a9de2-a1fc-447e-b36d-3ac90e0bca10
- http://www.fairbankscd.org/files/treatment%20gap(1).jpg
- http://www.soros.org/publications/closing-addiction-treatment-gap-early-accomplishments-three-year-initiative
- http://www.casacolumbia.org/templates/PressReleases.aspx?articleid=680&zoneid=95